Ventricular Septal Defect (VSD)
A ventricular septal defect is one or more openings in the interventricular septum, producing a shunt between ventricles. Large defects result in a significant left-to-right shunt and produce dyspnea with feeding and poor growth. A loud, harsh, holosystolic murmur at the lower left sternal border is common. Recurrent respiratory infections and heart failure may develop. Diagnosis is by echocardiography. Defects may close spontaneously during infancy or require surgical repair. Endocarditis prophylaxis is recommended.
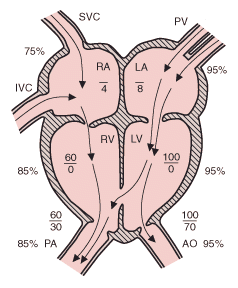 Ventricular septal defect (VSD) is the 2nd most common congenital heart anomaly after bicuspid aortic valve, accounting for 15 to 20%. It can occur alone or with other congenital anomalies (eg, tetralogy of Fallot, complete atrioventricular septal defects, transposition of the great arteries).
Ventricular septal defect (VSD) is the 2nd most common congenital heart anomaly after bicuspid aortic valve, accounting for 15 to 20%. It can occur alone or with other congenital anomalies (eg, tetralogy of Fallot, complete atrioventricular septal defects, transposition of the great arteries).
VSDs are classified by location: membranous (perimembranous), trabecular muscular, outlet (supracristal or subpulmonary), or inlet defects. Membranous defects (70 to 80%) involve varying amounts of muscular tissue adjacent to the membranous septum (thus called perimembranous defects); the most common type occurs immediately below the aortic valve. Trabecular muscular defects (5 to 20%) occur in the middle portion of the muscular septum. Outlet defects (5 to 7% in the US; about 30% in Far Eastern countries) occur in the ventricular septum under the pulmonary valve. Inlet defects (5 to 8%) occur posterior to the septal leaflet of the tricuspid valve.
Magnitude of the shunt depends primarily on defect size; larger defects result in a larger left-to-right shunt. Over time, a large shunt causes pulmonary artery hypertension, elevated pulmonary artery vascular resistance, right ventricular pressure overload, and right ventricular hypertrophy. Ultimately, the increased pulmonary vascular resistance causes shunt direction to reverse (from the right to the left ventricle), leading to Eisenmenger's syndrome Small defects produce a relatively small left-to-right shunt; the pulmonary artery pressure is normal or only slightly increased. Heart failure (HF) and Eisenmenger's syndrome do not develop.
Symptoms and Signs
Symptoms depend on defect size and magnitude of the left-to-right shunt. Children with a small VSD are typically asymptomatic and grow and develop normally. In those with a larger defect, symptoms of HF (eg, poor weight gain, fatigue after feeding) appear at age 4 to 6 wk. Frequent lower respiratory tract infections may occur. Eventually, untreated patients may develop symptoms of Eisenmenger's syndrome.
Small VSDs typically produce a grade 3 to 4/6 holosystolic murmur (with or without thrill) at the lower left sternal border; it is audible shortly after birth. The precordium may be mildly hyperactive, but S2 is normally split and has normal intensity.
Larger VSDs produce a similarly loud holosystolic murmur that is present by age 2 to 3 wk. S2 is usually narrowly split with an accentuated pulmonary component. An apical diastolic rumble (due to overflow through the mitral valve) and findings of HF (eg, tachypnea, dyspnea with feeding, gallop, crackles, hepatomegaly) may be present.
Diagnosis
Diagnosis is suggested by clinical examination, supported by chest x-ray and ECG, and established by echocardiography.
If the VSD is large, chest x-ray shows cardiomegaly and increased pulmonary vascular markings. ECG shows left ventricular hypertrophy or combined ventricular hypertrophy and, occasionally, left atrial hypertrophy. ECG and chest x-ray are typically normal if the VSD is small.
Two-dimensional echocardiography with color flow and Doppler studies establishes the diagnosis and can provide important anatomic and hemodynamic information, including the defect's location and size and right ventricular pressure. Cardiac catheterization is usually unnecessary.
Treatment
Small VSDs, particularly muscular septal defects, often close spontaneously during the 1st few years of life. A small defect that remains open does not require medical or surgical therapy.
If infants do not respond to medical treatment or have large shunts (with pulmonary to systemic flow ratio ≥ 2:1), surgical repair may be done during the 1st few months of life. Current surgical mortality rate is 2 to 5%. Surgical complications may include residual ventricular shunt, right bundle branch block, complete heart block, and ventricular arrhythmias.
http://www.merck.com/mmpe/sec19/ch287/ch287c.html#CIHCAHDJ



